Fishy Vaginal Odor: Causes, Management, and When to See a Doctor
I. Reader’s Question:
“Doctor, lately my private area has developed a fishy smell, especially after sex. I have washed thoroughly, but the smell won’t go away. Is this a sign of a disease? What should I do now?”
II. Answer from the Doctor/Expert:
1. Understanding Vaginal Odor and Normal Changes
Vaginal odor is a natural and constantly changing part of a woman’s body, not a static indicator but a dynamic physiological sign. A healthy intimate area can have many different odors depending on the menstrual cycle, physical activity, diet, and other individual factors. For example, the smell can be slightly salty, sweet, or like copper/blood, or musk. These changes are completely normal and are not a sign of pathology. It is important for each individual to recognize their own “normal scent” so they can distinguish when an abnormal change occurs. A healthy intimate area usually does not have a strong or unpleasant odor, and vaginal discharge is often clear, milky white, or slightly off-white. If the intimate odor changes suddenly, becomes strong and unpleasant, especially a fishy smell, it may be a warning sign that needs attention. This change is not merely a matter of personal hygiene but often signals an imbalance in the natural microbial environment of the vagina.
2. Deep Causes and Factors Related to a Fishy Odor
A fishy odor in the intimate area is often a sign of an imbalance in the vaginal microbial system, a condition called bacterial vaginosis. This is a common problem that can be related to many factors.
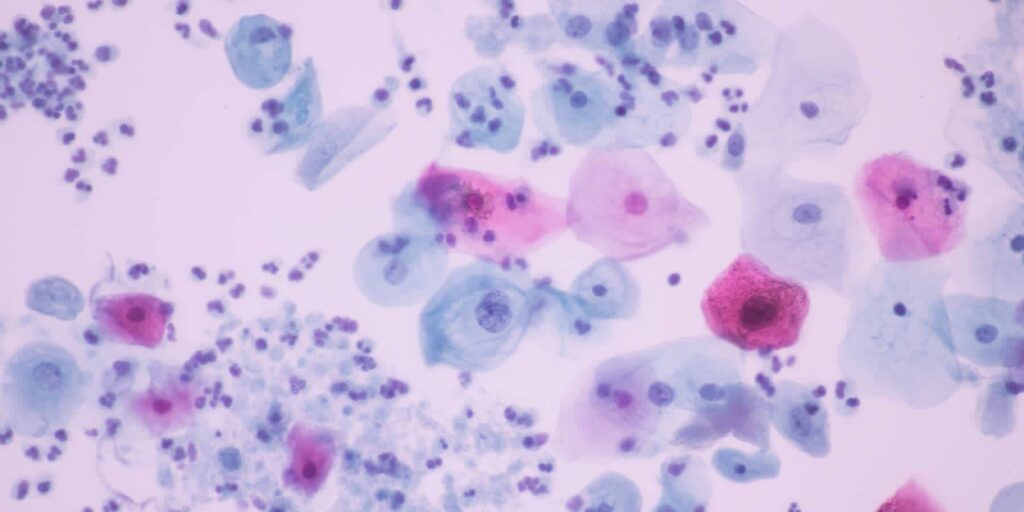
2.1. Bacterial Vaginosis (BV)
Bacterial Vaginosis (BV) is the most common cause of a fishy odor. This condition occurs when there is a severe imbalance in the natural microbial flora of the vagina. Specifically, the number of beneficial bacteria, mainly Lactobacilli (lactic acid-producing bacteria), is significantly reduced, while harmful anaerobic bacteria (such as Gardnerella vaginalis, species of Prevotella, Mobiluncus, and Mycoplasma hominis) overgrow. The mechanism that causes the fishy odor is that these anaerobic bacteria produce chemical compounds called volatile amines, including trimethylamine. These amines have a characteristic odor, like rotten fish. This smell often becomes more pronounced and stronger after sexual intercourse because semen is alkaline, which increases the pH in the vagina. This alkaline environment makes volatile amines more likely to evaporate, making the odor more unpleasant.
2.2. Trichomonas Infection (Trichomoniasis)
This is a sexually transmitted infection (STI) caused by the parasite Trichomonas vaginalis. In addition to a fishy odor, trichomoniasis is often accompanied by other symptoms such as green or yellow discharge, which may be frothy, along with itching and burning in the intimate area.
2.3. Common Risk Factors
Many factors can increase the likelihood of developing BV and intimate odor problems, and these factors often overlap with risk factors for other sexually transmitted infections (STIs). This indicates a complex link between sexual health and the vaginal microbiome, and BV may be an indicator of susceptibility to more serious STIs.
- Sexual Activity: Having multiple new or multiple sexual partners, as well as unsafe sexual intercourse (not using condoms), can alter the vaginal microbiome and increase the risk of BV and other STIs.
- Vaginal Douching: This is an unrecommended hygiene practice and is one of the main causes of vaginal microbial imbalance. Many people mistakenly believe that douching helps clean and eliminate odor, but in fact, this practice disrupts the natural pH balance and removes beneficial bacteria in the vagina. This removes protective bacteria and allows harmful bacteria to overgrow, leading to BV and other infections. Douching products often contain strong chemicals that can irritate vaginal tissue. This shows that the fishy odor is a warning sign of vaginal microbial imbalance, not just a simple hygiene issue, and seemingly “clean” practices like douching are the main cause of this imbalance.
- Intrauterine Device (IUD): Some studies suggest that IUD placement, especially the copper IUD, may increase the risk of developing BV.
- Smoking: Smoking is a significant risk factor for BV and is associated with a decrease in the number of beneficial Lactobacillus bacteria, while increasing vaginal pH.
- Improper Hygiene: Although not a direct cause, not changing underwear frequently, wearing tight, damp clothing can create a favorable environment for bacteria to grow and cause odor.
- Forgotten Tampon/Sanitary Pad: A tampon left forgotten in the vagina can cause a foul, unpleasant odor due to the accumulation of bacteria.
- Trimethylaminuria (Fish Odor Syndrome): In some very rare cases, a fishy odor may be due to a genetic condition where the body cannot properly metabolize trimethylamine (TMA). TMA accumulates and is excreted through sweat, urine, and vaginal secretions, causing a fishy odor.
3. Recognizing Symptoms and Differentiation
Recognizing symptoms is the first step to seeking medical support, however, the absence of clear symptoms (especially itching) or the overlap of symptoms between different conditions (BV vs. yeast infection) makes self-diagnosis extremely unreliable, emphasizing the necessity of professional medical diagnosis.
- Fishy Odor: This is the most characteristic symptom of BV, especially stronger after sexual intercourse and during menstruation. This smell is due to the volatile amines produced by anaerobic bacteria.
- Vaginal Discharge:
- BV: Discharge is usually grayish-white or off-white, thin, homogeneous, and may coat the vaginal walls. This is different from normal discharge (clear or milky white, odorless, changes with the cycle).
- Trichomoniasis: Discharge is usually green or yellow, frothy, and has a strong fishy odor.
- Other Symptoms:
- BV: Usually does not cause significant itching or burning, but some people may experience mild itching or irritation. There may be a burning sensation during urination. Notably, up to 84% of people with BV may not have obvious symptoms.
- Trichomoniasis: Often causes itching, burning, genital swelling, and pain during urination or intercourse.
- Yeast Infection (Candidiasis): Discharge is usually thick, white, like cottage cheese, often odorless or with a mild yeasty smell, and causes intense itching and burning.
- Differentiation: A strong fishy odor is the characteristic sign of BV, while a yeast infection usually has no odor or a yeasty smell, accompanied by intense itching and lumpy discharge. Although there are subtle differences between BV and yeast infection in terms of odor and discharge characteristics, the presence of itching in both conditions is a major factor of confusion for the patient, reinforcing why self-diagnosis is ineffective.
Table 1: Differentiating Normal and Abnormal Vaginal Discharge
| Characteristic | Normal Discharge | Abnormal Discharge |
|---|---|---|
| Color | Clear, milky white, or slightly off-white. | Grayish-white, dark yellow, green, brown, red (bloody). |
| Consistency/Texture | Changes with the cycle (liquid, sticky like egg whites around ovulation; thicker, slightly sticky toward the end of the cycle). | Thin like water, frothy, lumpy like cottage cheese, or pus. |
| Odor | Odorless or mild, not unpleasant. | Fishy, foul, strongly sour. |
| Accompanying Symptoms | No itching, no burning, no pain. | Severe itching, burning, swelling, redness, pain during urination, pain during intercourse, pelvic pain. |
4. Accurate Diagnosis: Why is a Doctor’s Visit Necessary?
Self-diagnosing intimate area problems is very difficult and often inaccurate. Symptoms can overlap between different conditions such as BV, yeast infection, Trichomoniasis, or other sexually transmitted infections (STIs). Incorrect treatment can worsen the condition or mask a more serious problem. Professional diagnosis not only accurately determines the cause of the odor but also differentiates between conditions with similar symptoms, preventing incorrect treatment and potential complications due to inaccurate diagnosis. The diagnostic process at a medical facility often includes the following steps:
- Clinical Examination and Medical History: The doctor will ask about current symptoms, medical history, and risk factors. A pelvic examination will then be performed to look for signs of infection, such as increased discharge or smelly discharge.
- Vaginal Swab: The doctor will use a speculum to take a small sample of vaginal discharge for laboratory testing.
- Diagnostic Tests:
- Wet Mount: The vaginal discharge is examined under a microscope to look for “Clue cells” – vaginal epithelial cells covered with bacteria, blurring their borders. This is a characteristic sign of BV.
- Vaginal pH Test: Measures the pH of the vaginal fluid. A healthy vaginal pH is normally between 3.5-4.5. A pH greater than 4.5 is a sign of BV or Trichomoniasis. However, the pH test cannot distinguish between these two conditions.
- Whiff Test: The doctor will add a drop of potassium hydroxide (KOH) solution to the vaginal sample. If a strong fishy odor is immediately noticeable (a positive “whiff” test), it is a strong sign of BV.
- Gram Stain and Nugent Score: This is considered the gold standard for BV diagnosis. This method quantitatively assesses different types of bacteria, including Lactobacillus and pathogenic microorganisms, on a stained slide of vaginal fluid.
- Nucleic Acid Amplification Tests (NAATs): More modern tests like NAATs can be used to detect the DNA of pathogenic bacteria (e.g., Gardnerella vaginalis) or parasites (Trichomonas vaginalis). These tests have high sensitivity and specificity, similar to or better than traditional tests, and are especially useful when wet mount is unavailable or results are unclear.
5. Effective Treatment Methods and Recurrence Management
5.1. Treatment for Bacterial Vaginosis (BV)
BV is treated with prescription antibiotics. Common and effective medications include:
- Metronidazole: Available as an oral form (500mg, twice daily for 7 days) or a vaginal gel (0.75% gel, 5g, once daily for 5 days). Oral metronidazole is often the preferred choice for non-pregnant individuals.
- Clindamycin: Available as a vaginal cream (2% cream, once daily for 7 days) or an oral form (300mg, twice daily for 7 days). An important note is that clindamycin cream can weaken latex condoms within 72 hours of use. Therefore, alternative contraception or abstinence from sexual intercourse is required during this time.
The most important treatment principle is to take the entire course of antibiotics as prescribed by the doctor, even if symptoms have disappeared. This ensures complete eradication of the pathogenic bacteria and significantly reduces the risk of recurrence.
5.2. Treatment for Trichomonas Infection (Trichomoniasis)
Trichomoniasis is also treated with antibiotics, usually a single 2g dose of Metronidazole or a single 2g dose of Tinidazole. For women, Metronidazole 500mg, twice daily for 7 days is also a recommended treatment regimen.
5.3. Managing BV Recurrence
BV recurrence is a complex and persistent problem, very common, with 50-80% of women experiencing recurrence within 6-12 months after completing antibiotic treatment. This condition is not only due to insufficient treatment but is also deeply related to bacterial biology, the incomplete recovery of the beneficial microbial flora after treatment, and partner factors. This requires a multidimensional and personalized approach to disease management. The main reasons for this high recurrence rate include:
- Reinfection from a Partner: Recent data, particularly from a randomized controlled trial at the Melbourne Sexual Health Centre (MSHC), suggests that treating the male partner simultaneously with the female partner with oral and topical antibiotics may significantly improve BV cure rates. However, previous studies had conflicting results on the efficacy of treating the male partner in preventing BV recurrence in the female partner. For female-female couples, simultaneous testing and treatment are also recommended due to the high rate of BV concordance, although more clinical research is needed for specific guidelines.
- Biofilm Persistence: BV-causing bacteria, especially Gardnerella vaginalis, have the ability to form a protective biofilm on the vaginal wall. This layer acts as a barrier, reducing the ability of antibiotics to penetrate and kill the bacteria, leading to the persistence of the pathogen and recurrence after clinical cure.
- Failure to Restore a Healthy Vaginal Microbiome: After antibiotic treatment, the vaginal microbiome is often dominated by Lactobacillus iners instead of more beneficial species like Lactobacillus crispatus or Lactobacillus jensenii. L. iners is associated with microbial instability, while L. crispatus is associated with microbial stability and health, so failure to restore a L. crispatus-rich bacterial community may be the main reason for recurrence.
- Antibiotic Resistance: Some strains of Gardnerella vaginalis have shown resistance to metronidazole and clindamycin, and resistance may increase after previous treatment courses, reducing the effectiveness of standard regimens.
5.4. Adjunctive and Emerging Methods for Recurrent BV
To cope with the high recurrence rate, researchers and doctors are exploring many adjunctive and emerging methods:
- Boric Acid: Often used as a vaginal suppository (e.g., 5g, twice weekly for 4 months) for recurrent BV. In vitro studies show that it can inhibit biofilm formation of some bacteria, and when used with antibiotics, may improve cure rates for recurrent BV. However, more research is needed on its long-term efficacy when used alone and its safety when used topically.
- Probiotics: The goal is to restore the vaginal microbiome with beneficial bacteria, especially Lactobacillus species. They can be taken orally or vaginally. However, evidence for the effectiveness of commercial products is limited, and many products contain Lactobacillus strains more common in the gut than the vagina. Some promising studies with vaginal L. crispatus (Lactin-V) have shown a significant reduction in BV recurrence.
- pH Adjustment: pH adjusters such as lactic acid or vitamin C aim to acidify the vaginal environment, reducing the growth of BV-causing bacteria. However, there is no reliable evidence that they are effective in treating BV alone or are better than existing antibiotics.
- Biofilm Disruptors: Research is looking for agents that can disrupt the biofilm, such as Astodrimer Sodium or Dequalinium chloride, which show potential in improving cure rates and reducing recurrence when used after antibiotics.
Table 2: Risk Factors for Bacterial Vaginosis (BV)
| Risk Factor | Description and Relation to BV |
|---|---|
| Sexual Activity | Having a new partner or multiple partners, unsafe sex (not using a condom), female same-sex relationships. |
| Vaginal Douching | Disrupts the vaginal microbial balance, eliminates beneficial bacteria, and increases the risk of infection. |
| Intrauterine Device (IUD) | Especially the copper IUD, may increase the risk of BV. |
| Smoking | Associated with a decrease in Lactobacilli bacteria and an increase in vaginal pH. |
| History of other STIs | Increases the risk of contracting BV. |
| Failure to restore beneficial flora after treatment | Especially the predominance of Lactobacillus iners instead of L. crispatus after antibiotic treatment. |
| Biofilm Persistence | BV-causing bacteria create a protective layer (biofilm) that reduces the effectiveness of antibiotics. |
| Diet | Deficiency in vitamins A, C, E, beta-carotene; a diet high in sugar and fat can affect the vaginal microbiome. |
6. Prevention and Home Care
Effective prevention is not about actively “cleaning” the vagina but about “maintaining and supporting the natural balance” of it, through behaviors that protect the microbiome rather than excessive intervention.
6.1. Proper Hygiene
- The Vagina is Self-Cleaning: The vagina naturally cleanses itself by secreting discharge and maintaining pH balance. There is no need to “wash” inside the vagina.
- Wash the Outside Only: Only wash the outside of the intimate area (vulva) with warm water and mild, unscented soap daily. Avoid using strong scented soaps or harsh detergents, as they can cause irritation and microbial imbalance.
- Absolutely No Vaginal Douching: This is the most important advice. Douching alters the natural pH and removes beneficial bacteria, increasing the risk of infection (BV, yeast, STI, PID) and other health problems such as infertility, ectopic pregnancy, and preterm birth. Douching does not permanently eliminate odor and can even worsen the condition.
- Avoid Scented Products: Limit the use of strongly scented feminine hygiene products such as deodorizing sprays, scented wipes, or scented sanitary pads/tampons, as they can cause irritation and microbial imbalance.
- Wipe from Front to Back: After using the toilet, always wipe from front to back to prevent bacteria from the anus from spreading to the vagina and urethra.
6.2. Healthy Lifestyle Supporting Intimate Health
- Safe Sexual Intercourse: Correct and consistent use of condoms is an effective measure to reduce the risk of BV and other STIs. Cleaning sex toys after each use is also very important.
- Choose Breathable Clothing: Wear cotton underwear and loose, breathable clothing to help keep the intimate area dry. A tight, damp, and stuffy environment creates favorable conditions for bacteria and fungi to grow. Change underwear daily and after exercise or excessive sweating.
- Balanced Diet: A balanced diet rich in green vegetables, fruits, and essential vitamins (A, C, E, D) can support vaginal health. Avoid foods high in sugar and fat, as they can negatively affect the microbiome.
- Quit Smoking: Smoking is a proven risk factor for BV and can negatively affect the vaginal microbiome, reducing the number of beneficial bacteria.
7. When to See a Doctor: Warning Signs
Intimate area symptoms, even if seemingly mild or familiar, can be signs of more serious conditions or can lead to significant complications if not treated promptly and accurately. Proactively seeking medical care is an important preventative action. You should visit a doctor if you notice any of the following signs, as they may indicate a condition requiring medical treatment:
- Abnormal intimate odor changes, especially a strong and persistent fishy smell that does not go away after a few days.
- Vaginal discharge changes significantly in color (grayish-white, green, dark yellow, brown, or bloody), consistency (thin like water, frothy, lumpy like cottage cheese), or the amount of discharge increases abnormally.
- Itching, burning, swelling, or pain in the vaginal or vulvar area.
- Pain or burning during urination.
- Pain or discomfort during sexual intercourse.
- Abnormal vaginal bleeding between periods, after sexual intercourse, or after menopause.
- Symptoms do not improve or worsen after trying home care measures or after a course of medication.
- You are pregnant and have any symptoms of BV, as BV during pregnancy can cause serious complications such as preterm birth.
- You suspect you may have a sexually transmitted infection (STI).
- You have been previously diagnosed and treated for BV, but symptoms recur continuously.
Table 3: When to See a Doctor
| Sign/Situation | Description |
|---|---|
| Abnormal intimate odor | Especially a strong and persistent fishy smell that does not go away after a few days. |
| Changes in discharge | In color (grayish-white, green, dark yellow, brown, or bloody), consistency (thin like water, frothy, lumpy like cottage cheese), or an abnormal increase in discharge volume. |
| Itching, burning, swelling, pain | In the vaginal or vulvar area. |
| Pain or burning during urination | Feeling uncomfortable when urinating. |
| Pain or discomfort during sexual intercourse | Experiencing inconvenience or pain during or after intercourse. |
| Abnormal vaginal bleeding | Between periods, after sexual intercourse, or after menopause. |
| Symptoms do not improve/worsen | After trying home care measures or completing a course of medication. |
| Pregnant and having BV symptoms | BV during pregnancy can cause serious complications such as preterm birth. |
| Suspecting an STI | Having risk factors or signs of a sexually transmitted disease. |
| Continuous BV recurrence | Previously diagnosed and treated for BV, but symptoms continue to return. |
8. Summary and Final Advice
A fishy odor in the intimate area is often a sign of an imbalance in the vaginal microbiome, most commonly Bacterial Vaginosis (BV) or Trichomoniasis. It is important to remember that the vagina is self-cleaning, and excessive intervention such as douching is not only ineffective but can also worsen the condition and increase the risk of infection. Self-diagnosis and treatment of intimate area problems are often inaccurate due to overlapping symptoms and the possibility of no clear symptoms. Therefore, always seek advice from a doctor or healthcare professional when there are any abnormal changes in odor, discharge, or other uncomfortable symptoms in the intimate area. Accurate diagnosis from an expert is key to an appropriate treatment method and preventing potential complications. To protect your intimate health, maintain proper hygiene (wash the outside only with warm water and unscented soap, absolutely no douching), practice safe sexual intercourse, and maintain a healthy lifestyle including a balanced diet and avoiding smoking. Proactive care and listening to your body is an important preventative action, helping to maintain the natural balance of the vaginal microbiome and overall health.
This article is written by Dr Đỗ Hữu Đạt. The doctor has many years of in-depth experience in reproductive and sexual health care.
Reference
[1]. Mayo Clinic. Vaginal health. Available from: https://www.mayoclinic.org/healthy-lifestyle/womens-health/in-depth/vagina/art-20046562
[2]. Centers for Disease Control and Prevention. Trichomoniasis. Available from: https://www.cdc.gov/std/treatment-guidelines/trichomoniasis.htm
[3]. Mayo Clinic. Vaginal discharge. Available from: https://www.mayoclinic.org/symptoms/vaginal-discharge/basics/causes/sym-20050825
[4]. Cleveland Clinic. Vaginal Discharge. Available from: https://my.clevelandclinic.org/health/symptoms/4719-vaginal-discharge
[5]. Healthline. What You Need to Know If Your Vagina Has a Fishy Odor. Available from: https://www.healthline.com/health/vaginal-health/what-you-need-to-know-if-your-vagina-has-a-fishy-odor
[6]. Intimate Rose. Why Does My Vagina Smell Like Fish? Available from: https://www.intimaterose.com/blogs/womens-health/fishy-vaginal-odor
[7]. WomensHealth.gov. Douching. Available from: https://womenshealth.gov/a-z-topics/douching
[8]. ResearchGate. Impact of Vaginal Douching on Women’s Health: Benefits and Potential Health Risk. Available from: https://www.researchgate.net/publication/377780613_Impact_of_Vaginal_Douching_on_Women’s_Health_Benefits_and_Potential_Health_Risk
[9]. Cleveland Clinic. Bacterial Vaginosis. Available from: https://my.clevelandclinic.org/health/diseases/3963-bacterial-vaginosis
[10]. American Academy of Family Physicians. Bacterial Vaginosis and Vulvovaginal Candidiasis. Available from: https://www.aafp.org/pubs/afp/issues/2018/0301/p321.html
[11]. Merck Manuals Professional Version. Bacterial Vaginosis (BV). Available from: https://www.merckmanuals.com/professional/gynecology-and-obstetrics/vaginitis-cervicitis-and-pelvic-inflammatory-disease/bacterial-vaginosis-bv
[12]. BCCDC. Bacterial Vaginosis. Available from: http://www.bccdc.ca/health-info/diseases-conditions/bacterial-vaginosis
[13]. Melbourne Sexual Health Centre. Bacterial Vaginosis Treatment Guidelines. Available from: https://www.mshc.org.au/health-professionals/treatment-guidelines/bacterial-vaginosis-treatment-guidelines
[14]. PMC. Current and Emerging Therapies for Bacterial Vaginosis. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC10264601/
[15]. Frontiers in Cellular and Infection Microbiology. The Vaginal Microbiome: A Dynamic Ecosystem Influenced by Host and Environmental Factors. Available from: https://www.frontiersin.org/journals/cellular-and-infection-microbiology/articles/10.3389/fcimb.2021.686167/full
[16]. Evvy. BV vs. Yeast Infection: What’s the Difference? Available from: https://www.evvy.com/blog/bv-vs-yeast-infection
[17]. Healthline. Bacterial Vaginosis vs. Yeast Infection. Available from: https://www.healthline.com/health/bacterial-vaginosis-vs-yeast-infection
[18]. PMC. Vaginal discharge: an approach to diagnosis and management in primary care. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC7905126/