Gonorrhea: Overview of What You Need to Know
1. What is Gonorrhea?
Gonorrhea is one of the most common sexually transmitted infections (STIs) worldwide and in Vietnam. Caused by the bacterium Neisseria gonorrhoeae, the disease can affect many parts of the body such as the genitals, anus-rectum, and throat. Failure to treat promptly can lead to serious and permanent complications. Gonorrhea is primarily transmitted through unsafe sexual contact. This bacterium can infect moist mucous membranes in the body, including:
- The urethra (the urinary tract – the tube that carries urine out of the body)
- The cervix (in women)
- The rectum
- The throat
- The eyes (less common, usually due to self-inoculation from the hands or mother-to-child transmission during birth)
Gonorrhea remains a major global public health challenge, with millions of new infections recorded each year.
- According to the World Health Organization (WHO), an estimated 82.4 million new gonorrhea infections occurred globally in adults aged 15–49 years in 2020. [1]
- In the United States, according to data from the U.S. Centers for Disease Control and Prevention (CDC), more than 600,000 gonorrhea cases were reported in 2023. [2]
- The European Union/European Economic Area (EU/EEA) reported 46,728 confirmed gonorrhea cases from 27 countries in 2021, according to the European Centre for Disease Prevention and Control (ECDC). [3]
- Meanwhile, the Western Pacific region, of which Vietnam is a part, recorded an estimated 23.2 million new gonorrhea cases in 2020, according to WHO estimates. [4]
- In the densely populated area of Ho Chi Minh City, reports show an increase over the years, with nearly 2,000 cases recorded in 2023. [5]
2. Routes of Gonorrhea Transmission
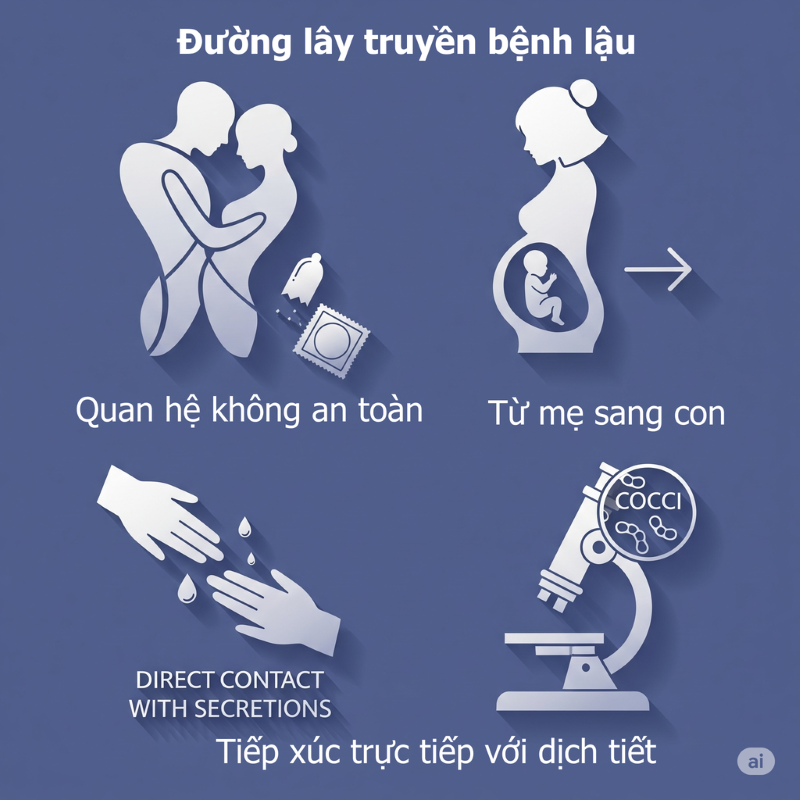
Gonorrhea is primarily transmitted through unsafe sexual contact with an infected person. The main routes of transmission include:
- Vaginal, Anal, or Oral Sex: These are the most common routes of infection, leading to gonorrhea in the genitals, rectum, or throat.
- Mother-to-Child: Pregnant women with gonorrhea can transmit the bacteria to their baby during childbirth, causing severe eye infection (gonococcal conjunctivitis) in newborns, which can even lead to blindness if untreated.
- Direct Contact with Secretions: Although rarer, direct contact with infected secretions (e.g., infected hands touching the eyes), or a scraped mucous membrane can also cause infection.
3. Signs and Symptoms of Gonorrhea
Gonorrhea infection often has no obvious signs and symptoms. This makes early diagnosis and infection control difficult and can still cause serious complications even without any symptoms. Symptoms usually appear 3 to 5 days after infection, which can be earlier in men and later in women. However, they can also take 14–30 days after exposure to the bacteria.
3.1. Signs and Symptoms of Gonorrhea in Women
Women often do not have any signs and symptoms or have mild symptoms that are easily confused with other vaginal or bladder infections. Symptoms may include:
- Pain or a burning sensation when urinating (dysuria, stinging)
- Increased vaginal discharge: The discharge may be yellow or green and have a foul odor.
- Abnormal vaginal bleeding: Bleeding between periods, after sexual intercourse, or heavier than usual menstrual flow.
- Pain in the lower abdomen or pelvic area.
- Pain during sexual intercourse (dyspareunia).
3.2. Signs and Symptoms of Gonorrhea in Men
In men, symptoms are usually more pronounced than in women, but may also be asymptomatic. Common symptoms include:
- Pain or a burning sensation when urinating (dysuria, stinging): This is one of the earliest and most common symptoms.
- Discharge from the penis: Usually white, yellow, or green, thick, and containing pus.
- Pain or swelling in the testicles: Less common, usually only affecting one testicle (epididymitis).
- Itching or discomfort at the urethral opening (urethritis): The urinary tract and meatus are swollen, red, itchy, and may have pus and mucus discharge.
- Pain during erection and sexual intercourse, painful ejaculation, possibly with blood in the semen.
3.3. Rectal and Pharyngeal Gonorrhea Symptoms
Gonorrhea in the rectum in both men and women through anal sex may not cause any symptoms or may manifest symptoms such as:
- Anal, rectal discharge.
- Itching, burning pain in the anal area.
- Rectal bleeding.
- Pain during defecation.
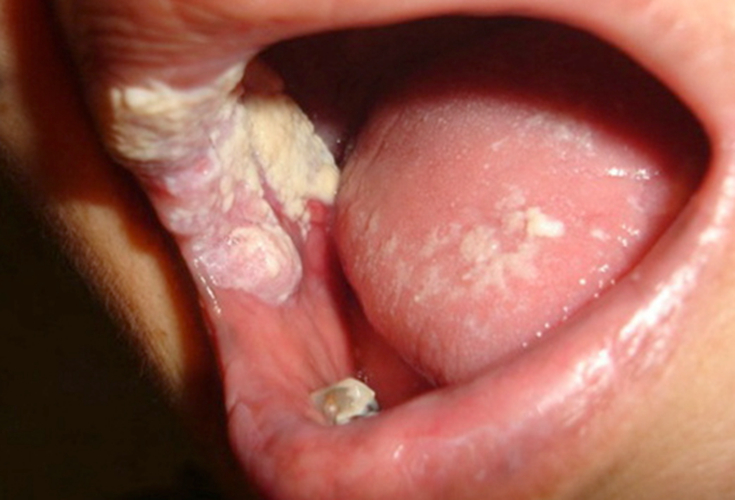
Gonorrhea in the throat is often the result of oral sex. Similar to rectal gonorrhea, pharyngeal gonorrhea is usually asymptomatic. If symptoms do occur, they are often very mild and may include:
- Soreness, itching, or a burning sensation in the throat, sometimes with swollen lymph nodes in the neck.
- Pharyngitis.
4. Risk Factors
Factors that significantly increase the risk of contracting Gonorrhea include:
- Having multiple or new sexual partners: A higher number of partners or new partners with an unknown sexual history will increase the risk of exposure to an infected person.
- Inconsistent and correct condom use: Condoms are an effective measure to prevent the transmission of Gonorrhea.
- A history of other sexually transmitted infections (STIs): Having had other STIs may increase the likelihood of contracting Gonorrhea.
- Sexual contact with a partner known or suspected to have Gonorrhea.
5. Complications
If not diagnosed and treated promptly, Gonorrhea can cause serious and permanent complications, affecting reproductive and systemic health.
- In women, untreated Gonorrhea can cause Pelvic Inflammatory Disease (PID)
- The infection can spread to the uterus, fallopian tubes, and ovaries, causing complications such as:
- Infertility: Due to the formation of scar tissue that blocks the fallopian tubes and can permanently damage them, preventing the egg from meeting the sperm.
- Ectopic pregnancy: A fertilized egg develops outside the uterus, which can be life-threatening.
- Chronic, persistent abdominal/pelvic pain.
- The infection can spread to the uterus, fallopian tubes, and ovaries, causing complications such as:
- In men:
- Epididymitis: Infection of the tube that carries sperm from the testicles, causing pain and swelling. In some cases, this can lead to infertility.
- Urethral Stricture: Chronic infection can cause scarring and narrowing of the urethra, leading to difficulty urinating.
- Also in both men and women:
- Disseminated Gonococcal Infection (DGI): The Gonorrhea bacteria can enter the bloodstream and spread throughout the body, causing joint infection (septic arthritis), skin infection (skin lesions, rash), heart infection (endocarditis), or brain infection (meningitis). DGI is a serious condition that can be life-threatening.
- Increased risk of HIV infection: Gonorrhea increases the likelihood of contracting or transmitting HIV.
- In newborns:
- Gonococcal Conjunctivitis: Due to transmission from an infected mother to the baby during birth, manifesting as pus discharge from the eyes and swollen eyelids. If untreated, it can lead to corneal ulceration, scarring, and blindness.
6. Diagnosis
Gonorrhea diagnosis is usually performed through laboratory tests. Common methods include:
- Nucleic Acid Amplification Tests (NAATs): Of these, PCR is the currently common test.
- This is a new technique with the highest sensitivity and specificity (accurate detection and identification capability), making it the priority test for detecting gonorrhea in symptomatic or asymptomatic patients. Results are also available quickly. The specimen can be collected from various sources such as: urine, or discharge from the urethra (in men), cervix (in women), rectum, or throat using a swab. PCR also allows for the simultaneous detection of multiple other STI agents.
- Bacterial Culture:
- This method requires a good specimen collection, timely inoculation into an appropriate culture medium, correct transportation, and incubation in an appropriate environment to achieve optimal results. Therefore, it may have limitations if not performed well. The site of specimen collection with the highest positive rate in men is the urethra, and in women is the cervix, which limits the source of specimens compared to the PCR method. Results take longer. However, this method allows for the identification of the presence of bacteria and the performance of antibiotic susceptibility testing (antibiogram), which is especially important in the context of increasing drug resistance and for cases that do not respond to initial treatment or have complex, recurrent gonorrhea.
7. Treatment
Gonorrhea can be cured with antibiotics. However, due to increasing antibiotic resistance, full testing is required, and strict adherence to the doctor’s prescription is essential. Important notes on treatment:
- Do not self-treat: Self-medication or non-adherence to the regimen can lead to treatment failure and increased risk of drug resistance.
- Partner Treatment: All sexual partners within 60 days before diagnosis also need to be tested and treated to prevent reinfection and spread of the disease.
- Avoid Sexual Intercourse: Patients should abstain from all sexual activity for at least 7 days until both they and their partner have completed treatment and the symptoms have completely disappeared.
- Follow-up Testing: Follow-up testing should be done after completing the treatment regimen to evaluate its effectiveness. Testing for other STIs like Chlamydia, Syphilis, and HIV should also be considered.
8. Prevention
Gonorrhea prevention is key to controlling the spread of the disease and protecting individual health. Effective prevention measures include:
- Practicing safe sex:
- Consistent and correct condom use: This is the most effective measure to prevent the transmission of Gonorrhea and other STIs during vaginal, anal, or oral sex.
- Limit the number of sexual partners and avoid sex with new partners of unknown history: Reducing the number of partners will reduce the risk of exposure to an infected person.
- Timely testing and treatment:
- Regular STI testing: If you have multiple partners or are at high risk, get tested for STIs regularly, including Gonorrhea.
- Immediate treatment: If you or your partner are diagnosed with Gonorrhea, seek immediate treatment and adhere to the doctor’s regimen.
- Education and awareness:
- Open discussion with your partner: Discuss your STI history and testing before sexual intercourse.
- Raise awareness of sexual health: Understanding STIs and how to prevent them is very important.
- Other measures:
- Avoid sharing needles: For people who inject drugs, do not share needles.
- Get vaccinated against HPV and Hepatitis B: Although these do not directly prevent Gonorrhea, these vaccines help protect against other STIs.
This article is written by BS. CKI. Võ Nguyễn Duy Hoà, a specialist in General Surgery, Urology, and Andrology, to provide fundamental knowledge about Gonorrhea, its transmission methods, recognizable signs, the importance of early diagnostic testing and treatment, as well as effective prevention. It helps you understand correctly to proactively protect your health and the community.
Reference
- [1]. Gonorrhoea (Neisseria gonorrhoeae infection). https://www.who.int/news-room/fact-sheets/detail/gonorrhoea-(neisseria-gonorrhoeae-infection
- [2]. National Overview of STIs in 2023 | STI Statistics | CDC. https://www.cdc.gov/sti-statistics/annual/summary.html
- [3]. Gonorrhoea – Annual Epidemiological Report 2021 – ECDC https://www.ecdc.europa.eu/sites/default/files/documents/gonorrhoea-annual-epidemiological-report-2021_0.pdf
- [4]. Quyết định 5165/QĐ-BYT 2021 hướng dẫn chẩn đoán và điều trị https://thuvienphapluat.vn/van-ban/Tai-nguyen-Moi-truong/Quyet-dinh-5165-QD-BYT-2021-huong-dan-chan-doan-va-dieu-tri-benh-Lau-494081.aspx
- [5]. TPHCM: Ghi nhận hơn 38.000 ca mắc loại bệnh tình dục nguy hiểm trong 1 năm – Dân trí https://dantri.com.vn/suc-khoe/tphcm-ghi-nhan-hon-38000-ca-mac-loai-benh-tinh-duc-nguy-hiem-trong-1-nam-20241211001845069.htm
- [6]. About Gonorrhea. https://www.cdc.gov/gonorrhea/about/index.html
- [7]. Sexually Transmitted Infections Treatment Guidelines, 2021. https://www.cdc.gov/std/treatment-guidelines/STI-Guidelines-2021.pdf
- [8]. Updated recommendations for the treatment of Neisseria gonorrhoeae, Chlamydia trachomatis and Treponema pallidum (syphilis), and new recommendations on syphilis testing and partner services. https://iris.who.int/bitstream/handle/10665/378213/9789240090767-eng.pdf?sequence=1